The following article is part of the Culture, Medicine & Psychiatry March 2024 special issue, “Student Experiences of Covid-19 around the Globe: Insights from the Pandemic Journaling Project” which is guest edited by Heather M. Wurtz, Katherine A. Mason, and Sarah S. Willen.
This special issue explores how the Covid-19 pandemic has impacted the mental health and wellbeing of high school and college students in diverse locations around the world. The collection analyzes data collected by the Pandemic Journaling Project, a combined research study and online journaling platform that ran on a weekly basis from May 2020 through May 2022, and from complementary projects. Contributions draw on a range of data including PJP journal entries, semi-structured interviews with PJP participants, autobiographical writing by students, and conversations about engagement with PJP in classroom and community-based settings. This week we feature a brief blog post by the authors of “The Eschucha (Listen) Podcast Project: Psychosocial innovation for marginalized Mexican youth and young adults”.
This article is by:
Cristopher Bogart Márquez Rodríguez, Master’s student in Psychosocial Intervention, Department of Psychology, Catholic University of Colombia
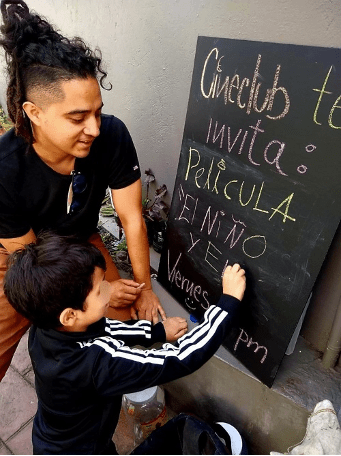
What is your article “The Eschucha (Listen) Podcast Project: Psychosocial innovation for marginalized Mexican youth and young adults” about?
The “Escucha” (Listen) Podcast Project” describes an innovative intervention project based in Mexico City, which sought to provide psychosocial support for young people in contexts of social exclusion. Youth participation in the project entailed weekly journaling with the Pandemic Journaling Project (PJP) — an online journaling platform and research study. Youth also engaged in weekly phone conversations with a member of the intervention team to give youth a space to express themselves and reflect on their lives and experiences. Regular and frequent communication with youth participants throughout the project helped foster a sense of trust towards the intervention practices and the intervention team. The project culminated in the creation of a podcast, in which each participant created a 2-5 minute chapter for the podcast about their experiences during the pandemic.
Tell us about how this project came to fruition.
Violence in Mexico has grown exponentially in recent years; one of the population sectors hardest hit by increasing violence is young people — especially those who live and coexist in contexts where violence is the daily norm. This sector is particularly vulnerable to different types of risks linked to material conditions and poverty. Despite increased need, there is a lack of emotional and therapeutic support programs that operate in marginalized communities. In my experience of around 13 years working with vulnerable groups, acting early can help prevent the reproduction of violent behavior. One of the objectives when intervening within these communities is to trigger cognitive processes that promote critical perspective of structural inequity, help youth reevaluate their abilities and potential, and strengthen their self-esteem. Bringing together the easy-to-use, digital platform of PJP with our own psychosocial tools allowed us to engage youth in these cognitive processes through dialogue, writing, and other creative outlets.
What was one of the most interesting findings?
One of our most interesting and important observations during the course of the project was the impact of the intervention on participants’ sense of wellbeing, as they described in both one-on-one conversations with team members, as well as in their journals. For young people who contend with overlapping forms of exclusion, it can be difficult to help them gain access to and engage in therapeutic spaces. But feeling truly listened to, for youth, can have a far-reaching effect. One of the project participants who had been incarcerated prior to the project and found the intervention particularly insightful, commented to an intervention team member: “If I had done something like this when I was younger, if someone had listened to me like this, with attention and without judging me, maybe my life would have been different.”
Who might be interested in reading your piece?
This article will be of interest to health professionals attracted by research and development of innovative, non-traditional projects aimed at young people in contexts of social exclusion.
If there was one takeaway or action point you hope people will get from this work, what would it be?
We can conclude by recognizing the impact of creatively-driven, contextually appropriate mental health interventions for youth. Socio-emotional work with young people in marginalized contexts in Mexico is not common, however, providing alternatives for support and professional accompaniment – as was done through this work – has made a notable difference in strengthening self-esteem among the youth participants.












